Trauma of ADHD Diagnoses
The Center for Disease Control (CDC) reports “approximately 11% of children 4-17 years of age (6.4 million) have been diagnosed with ADHD as of 2011.” That staggering number has risen at a rate of about 5% each year for almost a decade.
Where a family lives seems to effect the likelihood that ADHD is diagnosed and/or medicated. Nevada leads the country with the lowest prevalence of ADHD diagnoses for children between the ages of 4 to 17. On the other hand, Louisiana leads the country by medicating more than one in ten children for ADHD.
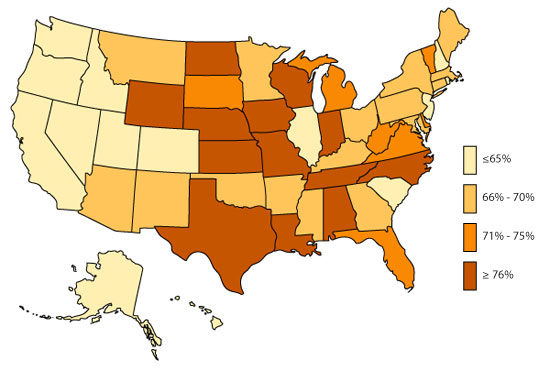
ADHD is a real medical issue, but, unfortunately, we do not know what precisely causes it. No single test exists to say that yes, a child absolutely has ADHD. Instead, doctors rely on a checklist of behaviors. Consider the diagnostic criteria for ADHD and consider how easy a 15-minute doctor visit can result in such a label.
ADHD-Inattentive Diagnostic Criteria
- Doesn’t pay close attention to details and/or makes careless mistakes
- Can’t pay attention for long periods of time either in schoolwork or play
- Doesn’t seem to pay attention when spoken to
- Seems to lose track of completing tasks
- Trouble organizing self to complete tasks
- Trouble staying focused and thinking through tasks
- Easily loses things
- Easily distracted
- Forgetful in everyday activities
NOTE: Not all the following criteria must be met in order for a diagnosis to be made; but the symptoms *must* be present in at least 2 different settings, such as school and home.
Not everyone believes that ADHD is truly growing at the reported rate. Sure, the diagnoses are increasing in number and more and more children are being medicated – but some people wonder: Are we dealing with a chronic misdiagnosing problem?
We know that some of the classic symptoms used to diagnose ADHD can be caused by other issues.
Executive Functioning Disorder leads to an array of disorganization, which can cause a child to lose track of completing tasks. Profoundly gifted children often have a hyper-focus on topics of interest, which allows them to be easily distracted and not hear when they are being spoken to. Sports-related concussions (diagnosed or not) can result in a mild traumatic brain injury, which will leave a person forgetful in everyday activities.
Recently, a resident doctor from inner-city Baltimore made an observation while working at Johns Hopkins Hospital.
[C]hildren diagnosed with ADHD also experienced markedly higher levels of poverty, divorce, violence, and family substance abuse. Those who endured four or more adverse childhood events were three times more likely to use ADHD medication.
Now, just because two factors seem to be related, we cannot jump to the conclusion that one factor automatically causes the other to happen. Instead, we have to try to answer the old chicken-or-the-egg question. Does ADHD and poorly managed behaviors lead adults to be less successful in their jobs, wind up living in poverty, and have children who also suffer from ADHD? Or, is it possible that living in poverty can somehow lead to the development of ADHD?
Dr. Nicole Brown, the Hopkins’ resident, thought it worthy to ask an entirely different question. She began with the astute observation that children living in poverty, surrounded by street and/or home violence, are in fact, suffering from a form of post-traumatic stress. Is it possible, then, that a segment of children are being misdiagnosed with ADHD because many of their PTSD behaviors look so much like inattention?
Adults and children suffering from PTSD experience a variety of symptoms as they cope to get past their trauma. These symptoms include:
- Recurring, intrusive memories. (May be seen as repetitive play or “daydreaming”)
- Nightmares and/or Flashbacks
- Irritable or aggressive behavior
- Self-destructive or reckless behavior
- Being extremely careful to not get hurt or in trouble
- Problems sleeping
- Poor self-image
- Blaming oneself for the traumatic event and its consequences
- Loss of interest in activities that were enjoyed prior to the trauma
- Strong emotional reactions to trauma triggers
- Feeling alienated from other people
- Hard time feeling happy or positive emotions
Nightmares, flashbacks, and recurring intrusive memories, for example, can cause extreme sleep problems. Even just one night’s lack of a good sleep can lead to distractibility and other problems. Compound that by weeks or months of restless sleep and it’s easy to see why children with PTSD have problems concentrating in a classroom.
We all dream of finding a quick fix for off-task behaviors. (If we’re truly honest with ourselves, some distractible kids are just downright annoying.) But, as parents and educational professionals, we owe it to our students to look past the behaviors we want to wish away and look deeply for what truly may be happening within a child.
Medicating the manifesting behavior may help a child become a more compliant student. But, looking deeply and addressing the core issue within a child will help them become a more functional and self-reliant human being.
Tell us what you think.
 |
 |
 |
 |




Yet finding a provider who is familiar with such therapy can be difficult for pediatricians and psychiatrists, Szymanski says. Though some hospitals have centers for childhood trauma, there isn’t a well-defined referral network. Even then, insurance companies, including the federal Medicaid program, may not always pay for the group sessions commonly used in parent training programs.